A Netflix-Like Disruption for Telemedicine
2020 has put us in situations that we had never thought we would experience. As if it were an apocalyptic Netflix production, we have had to spend months locked up at home, walking down the street with a mask, or writing an article like this from an office where there are no longer employees and the meetings are virtual.
In this same context, in recent months, health centres have experienced the paradox of being both overflowing with COVID patients (hospitals) and empty of their usual patients (outpatients). This has led to a telemedicine advance never seen to date.
The Role of Telemedicine
Telemedicine has played a crucial role during the toughest phase of this pandemic, experiencing a spectacular growth. The valuation of companies such as Teladoc Health (+ 265% valuation in 12 months) or Abi’s business growth (20% month-to-month during 2020) are a good reflection of this.
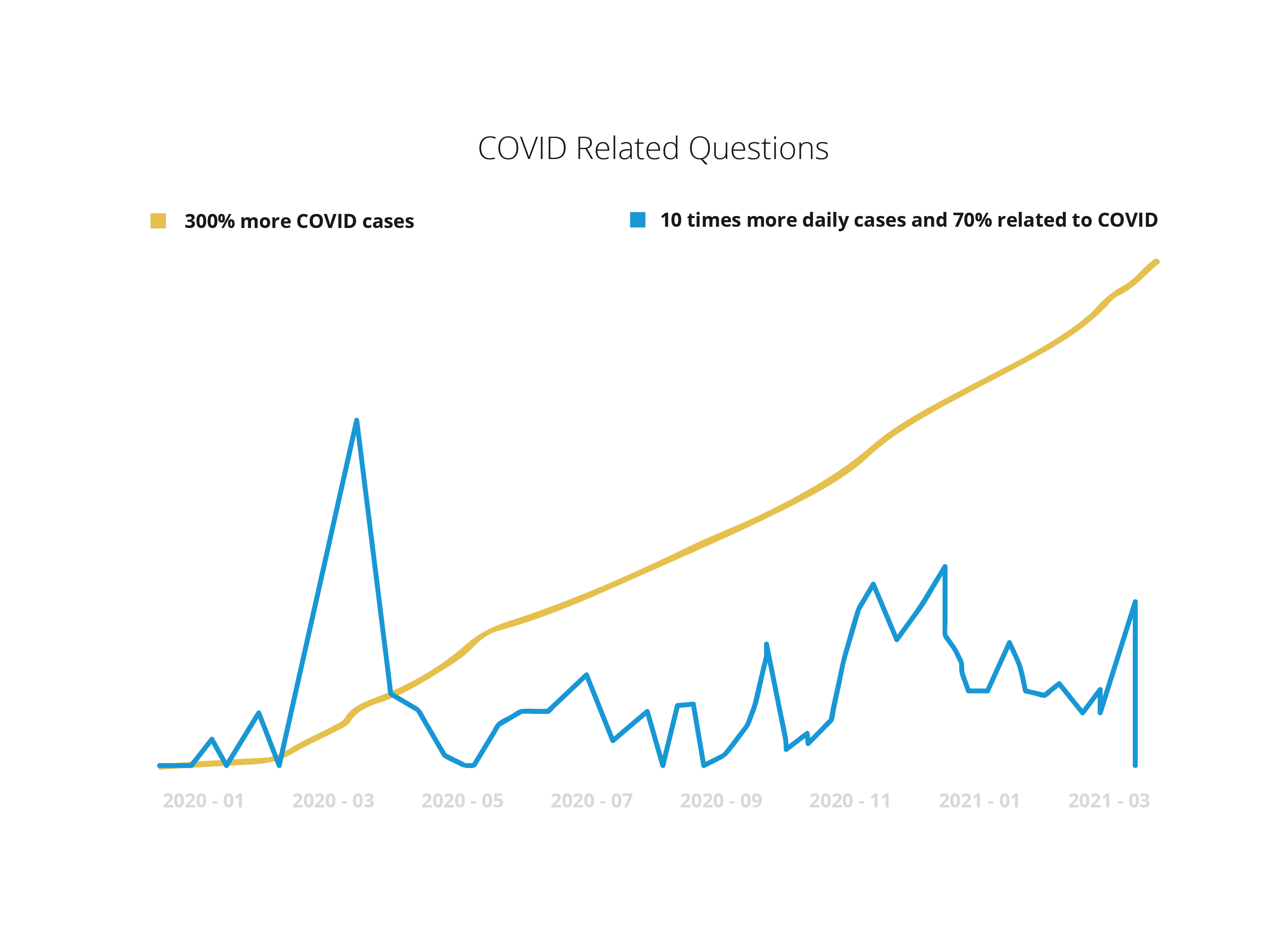
The analysis of Abi’s activity during 2020 is also very significant: 10 times more daily cases, 70% of the cases related to COVID at the peak (currently <10%) and 300% more non-COVID cases compared to early 2020.*[insert graph]
Not only did the use of our service massively increase due to COVID (users with symptoms or doubts about COVID), but also indirectly. In other words, people began to use Abi en masse as an alternative to going to the health centre in person, although their problems were not related to COVID. Our data is similar to those reported by other telemedicine companies. But the big question we all ask ourselves is whether this is a sustainable change, or a reflection of a specific situation.
A "Retro" Future for Digital Health
Since I started in digital health, more than 10 years ago, I’ve always find it paradoxical that even the most respected gurus of digital transformation (“The patient will see you now” – Eric Topol) saw the future of medicine in the form of a Blade Runner-style video conferencing in1982!
Likewise, now they talk about 5G and remote surgical operations as the great change that is about to come. These are solutions that, indeed, cover some needs, but are not likely to represent a true digital revolution. The reality is that, despite its growth during the pandemic, telemedicine is still carried out mostly through a XIXth-century invention: the telephone (90% in outpatient clinics in Spain, for example).
A Profound Change In Accessing Digital Health Services
The digital revolution in an economic sector is usually related to the disruption of the habits of people and companies due to the arrival of digital solutions that brutally displace those that previously existed: travel agencies, the entertainment industry or commerce in general, have experienced it. And, to put the example of commerce, the future was not in the form of a salesperson with a camcorder showing us clothes, but it was rather in the form of pictures, swipes, and extremely efficient purchase, shipping and return processes.
Medical video consultation, on the other hand, continues to require a programming, communication and organization system (visits are carried out every 15 minutes approximately), which makes it generate few efficiencies, beyond the fact that the user does not have to travel to see the doctor physically. Furthermore, doctors and patients still need to occupy the exact same amount of time (if not more), for a video consultation than for an in-person visit.
Doctors and patients still need to occupy the exact same amount of time, for a video consultation than for an in-person visit.
That is the reason why I do not believe that videoconferencing with a doctor represents the disruption that they have sold us, although of course it will have its place in the future of medicine.
A Massive Disruption for Digital Health
Disruption, in medicine, is having the doctor on your phone for whatever you need, without worrying about anything, planning or scheduling. This is how digital works, and right now, Google is providing 1 Billion answers to health questions every day, even though the consequences can be harmful for a lot of people.
In the same way that we have a courier service in our pocket (Glovo), a driver (Uber), a GPS assistant (Waze) or an online store (Amazon), having a doctor on your WhatsApp is the real revolution. Sending a photo and a text message and receiving a response from a doctor is truly competing with Google, which continues to perform at least 10 times more health consultations than all doctors in the world combined.
Having a doctor on your WhatsApp is the real revolution.
This is what we have done in Abi, where our users receive answers from doctors in 5 minutes, through the communication channels they use all the time (mainly WhatsApp, also SMS, Telegram, etc). Very interestingly, we find the impact of our micro-consultations to be similar to these of a video consultation: we are saving an in-person visit 70% of the times, but with a much higher utilisation than “traditional” telemedicine (> 50% annually on average, across 14 countries).
For us, this is disruption: Ease of use, efficiency and impact. Do you want to radically transform healthcare with us? Explore our innovative on-demand virtual care solutions and book a demo today.
Dr. Victor Vicens,Victor is the Chief Medical Officer and Co-Founder of Abi.As our Chief Medical Officer, Victor ensures the quality and breadth of the Abi healthcare professional network is world-class in all our local markets. Victor co-founded Abi based on insights gained from over 18 years of healthcare and digital transformation experience. His background includes practising roles as a resident physician & consultant psychiatrist. He is a veteran of previous medtech startups and has advised insurance and pharmaceutical companies on remote medicine and digital transformation. He holds medical degrees at undergraduate and masters levels, a Ph.D in neuroimaging, along with several publications in the field of psychosis and neuroimaging, and was a research fellow at Mount Sinai School of Medicine in NYU.


